Recent advancements in traditional Chinese medicine for COVID-19 with comorbidities across various systems: a scoping review
Background
Traditional Chinese medicine (TCM) has developed a rich theoretical system and practical experience in fighting to infectious diseases over the past thousands of years, and has played an important role in controlling the spread owing to its unique advantages. In particular, its significant contribution to the prevention and control of Corona Virus Disease 2019 (COVID-19) is widely recognized. COVID-19 infection is mainly non-severe with a favorable overall outcome, but patients with comorbidities tend to have a poor prognosis. However, a comprehensive review of TCM for preventing and treating COVID-19 with comorbidities across various systems is still lacking. Hence, this scoping review aims to conduct a comprehensive investigation on treatment outcome of TCM for treating COVID-19 with comorbidities across various systems.
Methods
The scoping review was conducted by searching English databases including PubMed and Web of Science, and Chinese databases including China National Knowledge Infrastructure and Wanfang between January 2020 and January 2024. We followed the inclusion and exclusion criteria to identify relevant literature. Information for inclusion in the literature were subsequently extracted and consolidated.
Results
We enrolled 13 literature that met the inclusion criteria in the review finally. Our analysis revealed that research on COVID-19 with comorbidities was mostly focused on circulatory diseases, including hypertension, heart failure, and cerebrovascular diseases, most common comorbidities were hypertension. Followed by endocrine and metabolic diseases such as diabetes, respiratory diseases including pulmonary tuberculosis and chronic obstructive pulmonary disease have been also addressed. However, there were few studies on co-infectious urogenital system disease, and no studies on the rheumatic, immune, hematological, nervous, reproductive, and skin systems diseases. Based on existing studies, TCM has significantly improved the clinical symptoms of COVID-19 with comorbidities such as fever, fatigue, dry cough, anorexia and asthma, the absorption of lung lesions, shortened the duration of viral shedding and the course of disease.
Conclusions
TCM has great application prospects in treating COVID-19 with comorbidities. These findings could provide important evidence for clinicians to treat COVID-19 with comorbidities. Multi-center studies are required to confirm our results in the future.
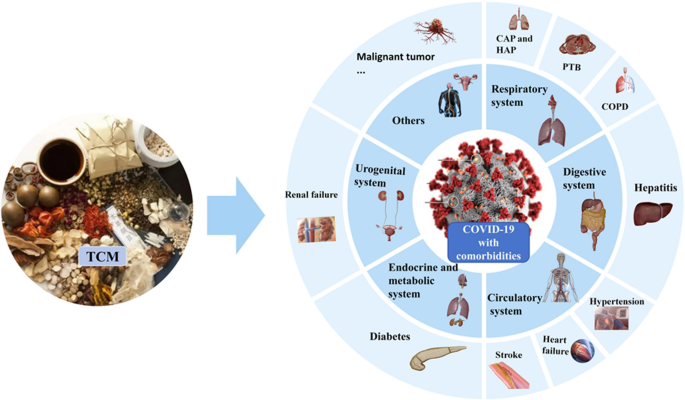
Graphical Abstract
Background
Traditional Chinese Medicine (TCM) has thousands of years in fighting infectious diseases and has played a vital role in epidemic control. Its significant contributions to the management of Coronavirus Disease 2019 (COVID-19) have been widely recognized [1,2,3,4,5,6]. The World Health Organization declared that COVID-19 is no longer a public health emergency of international concern on May 5, 2023. However, the threat of COVID-19 to humans persists with the severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) continues to mutate. For instance, there have been over 770 million cases and 7 million deaths globally. Notably, in the past 28 days (July 1 to July 28, 2024), there were over 200,000 new cases, 27,000 new hospitalizations, and over 3300 deaths [7]. While COVID-19 primarily presents as a non-severe illness with favorable prognosis, patients with comorbidities tend to have poorer outcomes. Studies indicated that the mortality rate among these patients can be as high as 65.9% [8]. Comorbidity refers to the clinical state in which one or more diseases coexist alongside the primary disease. Approximately 29.4% of COVID-19 patients have at least one comorbidity, and those with comorbidities experience more severe symptoms, increased rates of severe illness, and a higher risk of death compared with those without comorbidities [9,10,11,12,13,14,15].
Previous studies reported that TCM interventions, such as Qingfei Paidu decoction (QFPDD) and Maxing Shigan decoction were demonstrated good efficacy and safety in treating COVID-19 [16,17,18,19]. Additionally, TCM showed favorable treatment outcomes for COVID-19 patients with comorbidities such as chronic hepatitis B, cardiovascular and cerebrovascular diseases [17, 20]. However, no comprehensive review has been conducted on the role of TCM in the prevention and treatment of COVID-19 among patients with comorbidities across different systems. This knowledge gaps might limit the clinical application of TCM in managing COVID-19 with comorbidities. Therefore, it is urgent to conduct a comprehensive and systematic review of TCM’s efficacy in treating COVID-19 with comorbidities across various systems, thereby providing higher-level evidence to promote its clinical applications. In this study, we reviewed relevant literature and summarized the efficacy of TCM in treating COVID-19 patients with comorbidities affecting systems such as the circulatory, endocrine, metabolic, respiratory, and digestive systems. The findings aim to enhance the understanding of TCM's current situation in managing COVID-19 with comorbidities and provide further reference for clinicians to ensure rational applications.
Methods
Search strategy
In the present study, two reviewers independently searched the literature on COVID-19 with comorbidities across various systems using four databases, including two English-language databases such as PubMed (https://www.ncbi.nlm.nih.gov/pubmed/) and Web of Science (https://www.webofscience.com/), and two Chinese databases such as China National Knowledge Infrastructure (CNKI, https://www.cnki.net/) and Wanfang Data (https://www.wanfangdata.com.cn/), covering the period from January 1, 2020 to January 31, 2024. The structured search strategy combined the following MeSH terms and keywords: Huashi Baidu, HSBD, Xuanfei Baidu, XFBD, Jinhua Qinggan, JHQG, Lianhua Qingwen, LHQW, Xuebijing, XBJ, Qingfei Paidu decoction, Lung Cleansing & detoxifying decoction, Lung Cleansing detoxifying decoction, QFPDD, traditional Chinese medicine, TCM, oriental medicine, Chinese Medicine; COVID-19, covid 19, sars cov 2, SARS-CoV-2, coronavirus 2019, coronavirus disease 2019, Novel coronavirus, 2019-ncov; treatment, effective, effect, outcome, follow up, efficacy, therapeutic effect. The search terms used are listed in Additional file 1 (Table S1A–B).
Inclusion criteria and exclusion criteria
EndNote X9 (Clarivate, Philadelphia, USA) was used to remove duplicate articles. Then, the titles and abstracts of articles were read to filter out those not relevant to the research objectives. Full texts were carefully evaluated according to the following inclusion criteria: (1) the studies on TCM for COVID-19 with comorbidities; (2) the studies are clinical studies including randomized controlled trials (RCTs), non-RCTs, and case reports. The exclusion criteria were as following: (1) unobtainable in full text format; (2) the literature described complications of COVID-19; (3) the literature did not present treatment outcomes; (4) in cases of duplicate data or publications, only the one with the most complete data or the earliest publication was incorporated.
Classification of various disease systems
We defined the systems based on the reference of Systematic Anatomy (9th edition) [21] and categorized different diseases according to the International Classification of Diseases, Eleventh Revision (ICD-11) (https://icd11.pumch.cn/). In this review, we demonstrated various disease systems including circulatory system, endocrine and metabolic system, digestive system, respiratory system, and urogenital system.
Circulatory system
The circulatory system includes the cardiovascular system and the lymphatic system. The cardiovascular system consists of the heart, arteries, capillaries, and veins, while the lymphatic system is composed of lymphatic vessels, lymphatic tissues, and lymphatic organs. Diseases of the circulatory system generally include hypertension, coronary heart disease, and heart failure (HF).
Endocrine and metabolic system
The endocrine system comprises endocrine glands and tissues. Endocrine, nutritional, or metabolic diseases generally include diabetes, malnutrition, overweight or obesity, hypoparathyroidism, and hyperparathyroidism.
Digestive system
The digestive system consists of the alimentary canal and the digestive glands. Diseases of the digestive system commonly include viral hepatitis, autoimmune hepatitis, and non-alcoholic fatty liver disease.
Respiratory system
The respiratory system consists of the respiratory tract and lungs. Diseases of the respiratory system generally include bronchitis, chronic obstructive pulmonary disease (COPD), asthma, and pneumonia.
Urogenital system
The urinary system includes the kidneys, ureters, bladder, and urethra, while the reproductive system comprises the internal and external genitalia. The internal genitals consist of the gonads, reproductive ducts, and accessory glands, while the external genitals include the organs of coitus between the sexes. Diseases of the genitourinary system generally include renal failure and glomerular disease.
Quality assessment of included literature
The methodological quality of trials was assessed by two reviewers independently. RCTs were evaluated according to the Jadad scale, which consists of four items: randomization (0–2 points), double-blindness (0–2 points), and withdrawals (0–1 point). The scores were aggregated, with a total score of 0–1 indicating low quality, 2 indicating moderate quality, and 3–5 indicating high quality [22]. Non-RCTs were evaluated using the Methodological Index for Non-Randomized Studies (MINORS), which consists of 12 items, with a total score of 24. Scores were aggregated, where a total score below 8 points indicates low quality, 8–15 indicates moderate quality, and 16–24 indicates high quality [23]. The quality of case reports selected was assessed using the JBI Critical Appraisal Checklists, which consists of eight items [24].
Data extraction and analysis
All retrieved literature was processed using EndNote X9 (Clarivate, Philadelphia, USA). Two reviewers independently extracted data, which included comorbidities, interventions, study type (single-center or multi-center), adverse reactions, outcomes, composition of TCM, and the usage of each TCM. Any discrepancies in the data extraction were reviewed and verified, with discussions facilitated by a third reviewer.
Results
General characteristics of studies
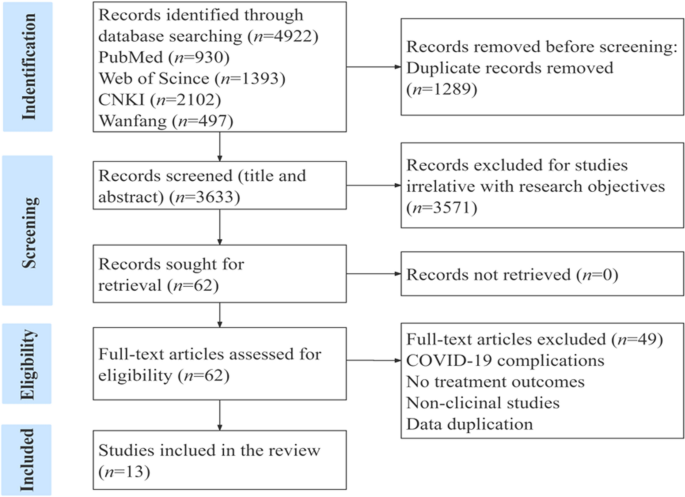
We retrieved 4922 records totally, including 2599 and 2323 literature from Chinese and English databases, respectively. After removing duplicates, the titles, abstracts and full text of 3633 records were screened. Finally, we enrolled 13 studies including 3 RCTs, 8 non-RCTs, and 2 case reports. Flowchart of the study was shown in Fig. 1. Detailed search strategies were shown in Additional file 1 (Table S1 A–B).
Fig. 1
Flowchart of the study
Characteristics of the studies enrolled were seen in Table 1. To clearly present the TCM treatment regimens for fighting COVID-19 with various comorbidities, we also compiled the composition details of each TCM formula, including their Chinese, English, Latin names, as well as the respective doses of these herbs (Additional file 2: Tab S2).
Table 2 Overview of COVID-19 with comorbidities
Additionally, we conducted a quality assessment to 13 studies included. An evaluation of the literature showed that none of the three RCTs reported the use of allocation concealment, two mentioned randomized grouping, however the specific method of randomization was not described in detail thus scoring 3, and 1 explicitly described the method of randomization thus scoring 4. Two cohort studies scored 18, and five out of six observational studies scored 12 due to the absence of a control situation, with the additional one item was scored as 14 because it reported on follow-up. As for two case reports, except for the item “Were adverse reactions or unexpected events detected and described?” was evaluated as “no”, the rest of the evaluation items were “yes”. We considered that the non-RCTs studies enrolled were high and moderate studies, and RCTs were high and low studies (Tables 3, 4and5).
COVID-19 with diseases of circulatory system
The circulatory comorbidities of COVID-19 mainly include hypertension, coronary heart disease, and cerebrovascular disease. A total of 12.1% of the studies indicated that 18.7% of COVID-19 patients had circulatory comorbidities [25], with higher mortality and ICU occupancy rates [26]. A retrospective cohort study showed that COVID-19 patients with cardiovascular and cerebrovascular diseases had better outcomes and significantly improved clinical symptoms (cough, fatigue, asthma, fever, dry cough, etc.) after TCM treatment (QFPDD), and lung CT imaging indicated absorption of pulmonary lesions in 92.5% of patients without serious adverse reactions [20].
Hypertension
Relevant studies indicated that hypertension is the most common comorbidity in COVID-19 patients, accounting for 45.8% [25], and is associated with adverse comprehensive outcomes, including death, ICU admission, and acute respiratory distress syndrome [27, 28]. In a study conducted among hospitalized COVID-19 patients in Iran, those with hypertension alone had a significantly higher mortality rate than those without comorbidities (20.8% vs. 12.7%) [29]. There are two clinical studies of TCM included in this disease.
A multicenter retrospective study showed that COVID-19 patients with hypertension received QFPDD in combination with Western medicine treatments (WMT) such as antiviral drugs, antibiotics. After six days of treatment, the clinical symptoms of different proportion such as fever and fatigue had been improved. 74.7% of the 99 cases with abnormal lung imaging results showed absorption of lung lesions; 99.2% (118/119) patients were cured and discharged. No serious adverse events occurred in all patients during hospitalization [16]. Li et al. found that the mean length of hospital stay for COVID-19 patients with hypertension was 10.8 ± 3.8 days, the mean systolic blood pressure decreased by 14.0 ± 5.7 mmHg, and the mean diastolic blood pressure decreased by 8.4 ± 2.5 mmHg using QFPDD with oxygen therapy and symptomatic supportive therapy without antiviral, anti-inflammatory, immune-modulating medications. These findings suggested that QFPDD could promote the negative conversion of SARS-CoV-2 RNA, facilitate the absorption of chest lesions, and help lower blood pressure in COVID-19 patients with hypertension [30]. Mihardja et al. demonstrated the efficacy and mechanism of acupuncture in the treatment of COVID-19 patients with hypertension and type 2 diabetes. The results indicated that acupuncture reduced blood pressure in patients with hypertension and lowered blood glucose and insulin resistance in patients with type 2 diabetes, suggesting that which might be a potential method to be used as an adjuvant therapy for such patients [31].
Coronary heart disease and heart failure
The proportion of COVID-19 patients with coronary heart disease (CHD) ranges from 10.7% to 15.6% [25]. Previous study showed that compared to COVID-19 patients without comorbidities, those with a history of CHD had a 1.45-fold increased risk of death, 1.57-fold increased risk of developing severe or critical cases, 1.75-fold increased risk of ICU/CCU admission [32], and up to 10.5% of the overall mortality rate [33]. Previous study reported that the combination of Yangyin Jiedu Mixture with fluid infusion and conventional treatment significantly improved the degree of chest pain in patients (total effective rate,100.0% vs. 87.5%) and enhanced the efficacy of electrocardiograms (total effective rate, 90.3% vs. 68.8%), and lower TCM syndrome scores after treatment (6.0 ± 1.6 vs. 7.8 ± 2.2) compared to conventional treatment alone. Furthermore, laboratory indicators such as IL-6, C-reactive protein, and the neutrophil-to-lymphocyte ratio showed significant improvement [34].
The proportion of COVID-19 patients with HF ranges from 4.3 to 24% [25, 35], and HF increases the risk of myocardial injury and death in COVID-19 patients [36]. Previous study predicted that 20 active compounds and 164 targets of Shenfu injection, which were mainly involved in three biological processes of metabolism, coagulation and cytokine signaling pathways in the immune system, and play an important role in the prevention and treatment of COVID-19 complicated with HF. It is suggested that Shenfu injection might be the potential to treat COVID-19 combined with HF [37]. In addition, there is one clinical study of TCM included in this disease. A RCT showed that compared to control group, BADUANJIN is as a traditional Chinese exercise that emphasizes a harmonious connection between mind and body through slow, coordinated, and sequential movements combined with modified Baoxin decoction and Yiqi Fumai freeze-dried powder had higher effective rate in the experimental group (54.2% vs 33.3%). Left ventricular ejection fraction (42.4 ± 6.7 vs. 37.7 ± 7.1) and left ventricular end-systolic diameter (3.8 ± 1.1 vs. 4.4 ± 1.0) were significantly improved in the treatment group compared to the control group [38].
Cerebrovascular diseases
The proportion of COVID-19 patients with cerebrovascular disease ranges from 1.0% to 1.9%, and cerebrovascular diseases increase the mortality rate of patients with COVID-19 [39]. A multicenter retrospective study reported that 96.3% of COVID-19 patients with stroke were treated by QFPDD, and 96.3% of patients were cured and discharged [40].
COVID-19 with diseases of endocrine and metabolic system
COVID-19 co-infected endocrine and metabolic diseases include diabetes, obesity, malnutrition, thyroid dysfunction, and hyperlipidemia, among them, the most common was diabetes. These comorbidities increase the risk of death in COVID-19 patients.
Diabetes
Studies indicated that 8.4–10.9% of COVID-19 patients had diabetes, which was the second most common comorbidity for COVID-19 [13]. The disease severity and mortality rate increased in COVID-19 patients with diabetes [41], with the mortality rate up to 7.8% [42]. A multicenter retrospective study showed that the number of fevers, cough and fatigue among COVID-19 patients with type 2 diabetes were significantly reduced at day 3 and day 6 during treatment compared to those before treatment, No serious adverse events occurred during treatment. All patients were cured and discharged from hospitals [43]. Tao et al. reported that Jingyin Gubiao decoction had significantly lowered TCM syndrome scores such as chills, sweating, expectoration, and cough (P < 0.05) [44]. Besides, Hu et al. showed that Anemarrhena asphodeloides Bunge, Astragalus membranaceus (Fisch.) Bge., Lonicera japonica Thunb., and Scutellaria baicalensis Georgi were high-frequency medicines for COVID-19, and showed favorable effect of blood-glucose control, suggesting that these TCM have a promising perspective for the treatment of COVID-19 with diabetes based on 120 Chinese herbal formulas analyzed [45]. Furthermore, previous studies demonstrated that the effective control of blood glucose with hypoglycemic agents such as metformin, insulin, DPP-4 inhibitors were conducive to reduce the incidence of complications and the risk of death in patients. Studies also showed that the earlier use of hypoglycemic agents, the better treatment outcome [41, 42, 46].
https://medical news today. com/recent-advancements-in-traditional-chinese-medicine-for-covid-19-with-comorbidities-across-various-system-a-scoping-review/